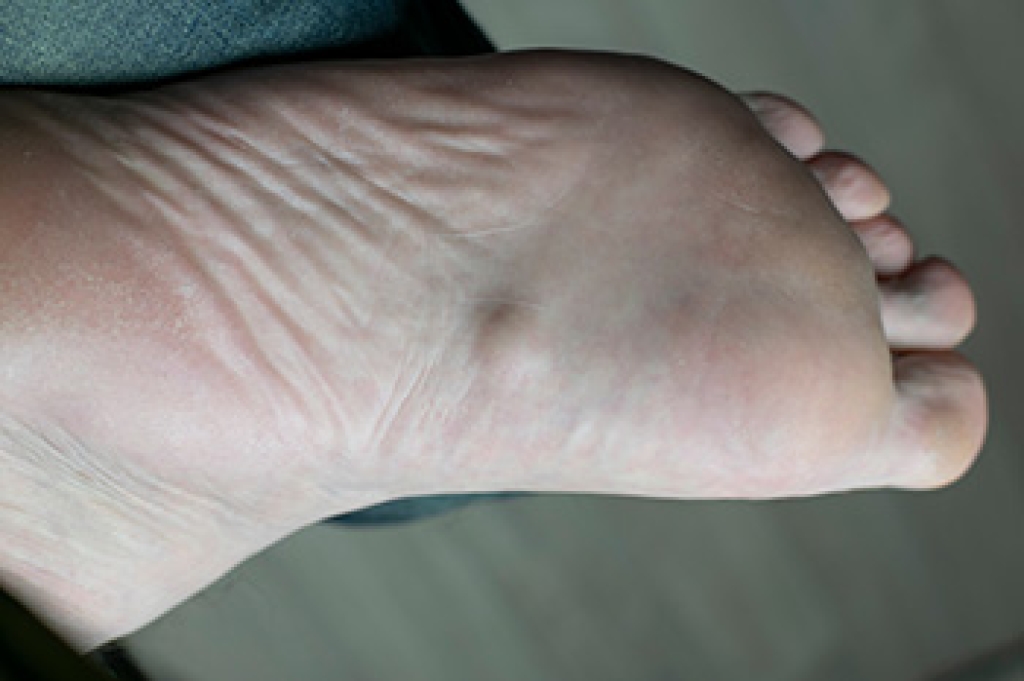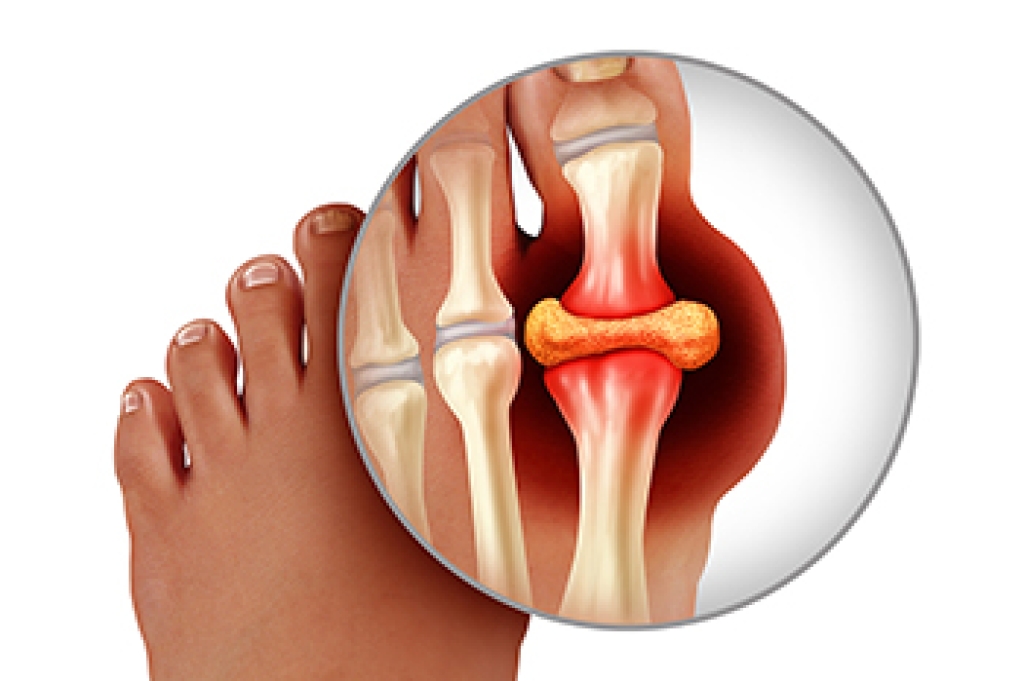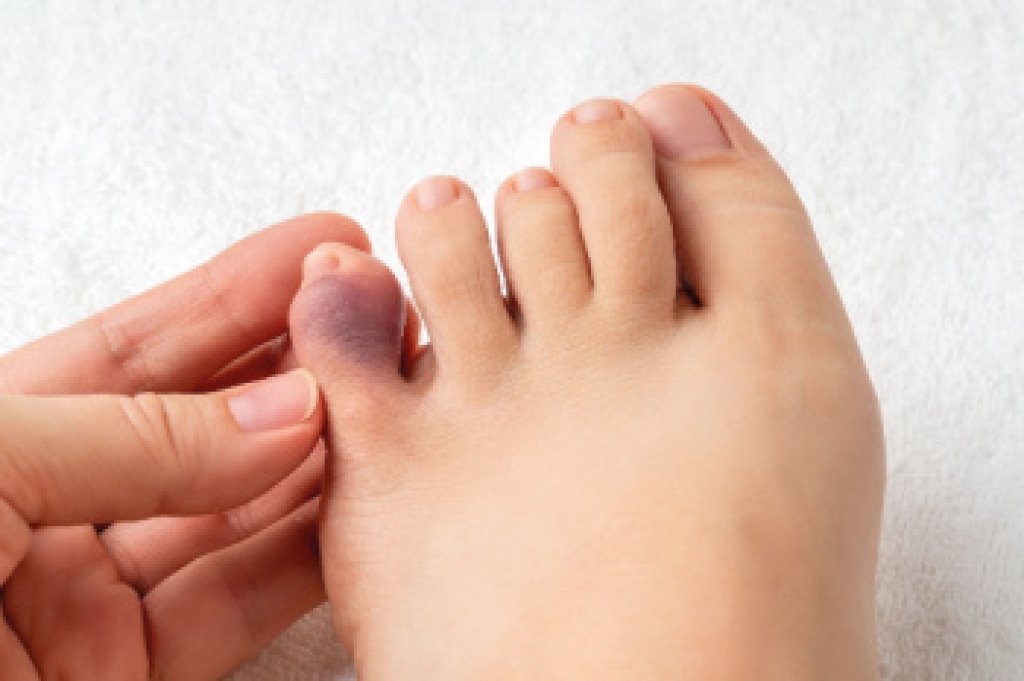
A broken toe is a common injury that can result from trauma, such as stubbing, dropping a heavy object on the foot, or sports related accidents. The toe may look swollen, bruised, or misaligned, and, in severe cases, it may appear deformed or out of place. It often feels painful, tender, or throbbing, particularly while walking, standing, or applying pressure. Additional symptoms can include difficulty in moving the toe, stiffness, or a cracking sensation at the time of injury. A podiatrist can begin by performing a thorough examination, assessing the degree of injury, and ordering imaging, such as X-rays, to confirm the break and identify any displacement. Treatment may involve buddy taping, protective footwear, pain management, or in more severe cases, surgical intervention to properly realign the bones. Because early professional care promotes healing, prevents complications, and restores mobility, it is suggested that you promptly schedule an appointment with a podiatrist for appropriate treatment solutions.
Broken toes may cause a lot of pain and should be treated as soon as possible. If you have any concerns about your feet, contact the podiatrists from Boston Common Podiatry. Our doctors will treat your foot and ankle needs.
What Is a Broken Toe?
A broken toe occurs when one or more of the toe bones of the foot are broken after an injury. Injuries such as stubbing your toe or dropping a heavy object on it may cause a toe fracture.
Symptoms of a Broken Toe
- Swelling
- Pain (with/without wearing shoes)
- Stiffness
- Nail Injury
Although the injured toe should be monitored daily, it is especially important to have a podiatrist look at your toe if you have severe symptoms. Some of these symptoms include worsening or new pain that is not relieved with medication, sores, redness, or open wounds near the toe.
If you have any questions please feel free to contact our office located in Boston, MA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.